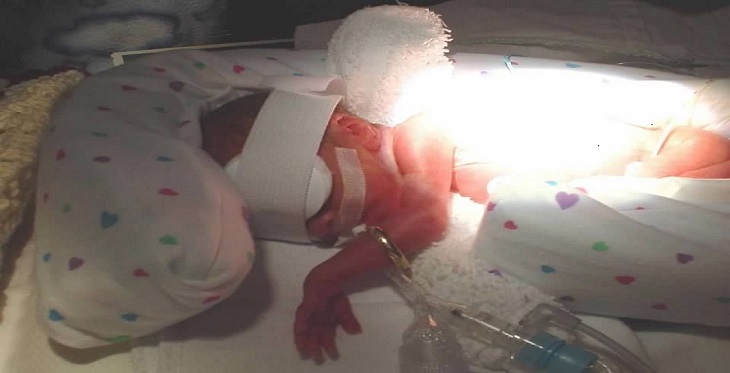
Imagine delivering a baby at 24 weeks gestation, or three months early. You deliver at the hospital closest to your house or the one that your OB/GYN recommends. Exploring the quality of care outcomes in that facility are not at the forefront of your mind. Wanting a healthy baby, or even a baby that simply survives, free of life-altering complications, becomes your goal. Quickly after this baby is born, he is whisked away to the neonatal intensive care unit (NICU), and it may be hours or sometimes even days before you see him again. The clinicians in that unit are trying their very best and they are providing excellent care: or are they? How do you know? Without questioning the intent or skill of clinicians, the data show that the quality of NICU care varies from unit to unit, and one complication in particular can vary widely: necrotizing enterocolitis (NEC). For this condition, there is a core of evidence-based prevention interventions that are essential to reduce the risk of contracting NEC. Perhaps most importantly among these tactics is giving baby the mom’s own milk, using a feeding protocol, limiting antibiotic and antacid exposure, and considering strategies for timely recognition. NEC-Zero is a prevention bundle for NEC and our team has made a concerted effort to share it freely so any unit in any location can deliver excellent care to any baby. However, improving quality is a difficult task, and it requires a committed team to implement the best evidence in the NICU.